“A surgeon with shaky hands under fear of violence and legal action cannot perform a successful operation and a quivering physician cannot administer medicine to his patient.”
According to the World Health Organization, between 8% and 38% of health workers suffer physical violence at some point in their careers.
Historically the healthcare worker, namely, doctor has played the three roles concurrently – “Healer,” “Teacher” and “Preacher” and enjoyed prestige in the community unlike any other profession. But slowly this image has been tarnished due to many factors including the profession itself. The craziness for easy money, commercial approach, earning fame at any cost, competitive attitudes, corruption, etc. has slowly encroached a section of this noble profession. Thus, a sense of distrust among the stakeholders and the common people has engulfed this stressful profession. As a downstream effect, since few decades attack on treating physicians, is taking an epidemic form in many countries like India. The seriousness of the attack regarding brutality has also become alarmingly life-threatening and has indeed taken and crippled lives of medical professionals. This has also resulted in temporary and mass interruption of duty by the doctors. Strike is a one of the nonviolent and legitimate forms of protest in a democracy, which is done collectively in mass mostly to get one or more demands to be fulfilled. It is well-known fact that the creamy layer of best students of the society chooses this profession and goes through a long period of training to become eligible for healthcare by regulatory body in India which is usually 10 years or more after school leaving examinations. Today, the safety of doctors both in public and private sectors has become a big issue as there are increasing reports of vandalism and mishandling of doctors at the hands of angry attendants of patients following any death or alleged medical negligence.
With the limitations of medical science, even in 21st century, it is impossible to save every patient even in the best of the hospitals in the world, and in India, a majority of the hospitals, mainly those run by the government are far from being best in the country, let alone in the world. Therefore, correlating any death of the patient with negligence of the doctor and violently reacting against him is not an expected human behavior, as aptly written“It can only be termed animal behavior when anyone attacks doctors.”
In the healthcare history, for the first time on 12th September 1978, elected representatives from 134 countries and 67 international organizations unanimously accepted “Alma-Ata Declaration” (of United Nations, UN),… “expressing the need for urgent action by all government, all health and development workers, and the world community to protect and promote the health of all the people of the world.” The Declaration had two core principles in it:
1. Health is a human right
2. In order to maintain the same, several social and economic sectors, in addition to health sector, needed to be actively involved and show results.
However, even after 40 years, we still are dreaming for “health for all.”
With a population of over 1.32 billion, India is well on its way to be world’s most populated country. Our population is on one hand our greatest strength and on the other greatest weakness. By 2020, the age of an average Indian will be about 29 years. While a young India is great for the industry and economy, the great Indian middle class is teetering on the brink of a major crisis – a healthcare crisis, one of the reasons being poor public funding. Healthcare system in India is based on public and private providers. India’s public healthcare system is a near disaster primarily due to the low funding. India’s per capita spending on healthcare is dismal. If we see the public funding as the percentage of gross domestic product (GDP), for the past 15 years, it has remained very low near 1.2%, nearly 20% of overall health expenditure in the country, with 80% being provided by private sector. Even in 2019–20 financial year, it has been only 0.98% of GDP.
In principle, government health services are available to all citizens under the tax-financed public system. In practice, bottlenecks in accessing such services compel households to seek private care, resulting in high out-of-pocket payments (69% of total expenditure). Alarmingly about 7% of our population is forced below the poverty line due to cost of healthcare.
Infrastructure – There are no global norms about the number of hospitals or number of beds for the number of populations. A report by World Health Organization (WHO) about the number of beds in South East Asia (SEA) region and the world average shows that between 2005 and 2012, the average number of beds in India was 9 beds per 10,000 population, while the world average was 30 per 10,000 population. Even SEA region also had an average of 11 beds per 10,000 population.
Manpower – What can be said about the comparison of India with Western world, even comparison to SEA region is also not very encouraging. A recent WHO report suggests that India is almost comparable to other countries of the region and even below than Maldives. While 44.6 global health workforce was suggested in 2016 for 10,000 population, India had nearly 29 per 10,000 population.
Public healthcare systems get their funds from the government, which makes it mandatory for them to cater to everyone. Hence, they are in no position to turn anyone away even if patients are penniless. As a result, people are forced to stand in long quies; many of them ultimately end up going to private healthcare providers for treatment and often face extreme financial challenges due to exuberant out-of-pocket expenses
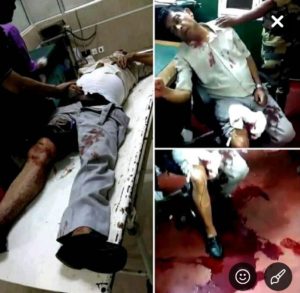
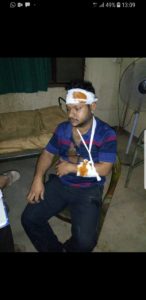
Whatever be the cause of violence, the impact is grievous. The loss of property or life clearly questions the current modalities and laws created for the protection of health sector from patients and their relatives. Since early 2017 till date, about 275 incidents of assault on doctors have been reported in West Bengal alone apart of numerous cases nationwide. Many of these have led to fatal injuries, disability and death too. Cases of verbal abuses, minor altercations, unreported cases and administrative terrorisms are not counted in these counts. The soft approach to people who target hospitals and health workers encourages potential assailants. Many times, it has been noted that political leaders often play partisan role to shield the perpetrators engaged in these violence rather than standing by the victims of the noble profession from the wrath of irresponsible care seekers, bystanders, or even unrelated hooligans as noted on national as well as local levels. Public should be educated to seek for legal action for professional misconduct on the part of doctor, if any. Interestingly this is the only profession which gives the beneficiary legal rights to seek grievance redressal in multiple foras for a single alleged misconduct of healthcare professionals. The existing state laws against violence in healthcare have mostly remained on papers only and rarely, if at all implemented. A Central law, supposed to be a stringent and deterrent one, as promised by the Union Minister of Health and family welfare supposed to be tabled in the winter session of the Parliament, 2019, have reportedly been stalled by the MHA citing reasons that no central legislation can be brought to protect the practitioners of one specific profession. This is amusing, to say the least, as there exist several legislations directed at the medical professionals alone. The profession which the policy makers “seva” at their convenience have been a part of Consumer Protection Act and may be further tightened in CPA 2019. What a dichotomy!
Last but not the least, if these types of relentless attack on this health-care profession is unchecked by the policy makers, political leaders, regulatory bodies and administrative authorities, then brilliant students will be scare to opt for this profession and the needs of the people in healthcare will be disregarded by the backbenchers of the school. Till about sometimes ago and off and on, now, the problem of violence in healthcare is also byproduct of sensational, unscientific and often biased media as the instigator of the widespread public distrust towards the medical fraternity.
Today’s residents are much wiser and more practical than before. For them every work in the hospital is a ladder on which they wish to go up and use that for their future life. Many of them are very clear about what they wish to do in future so they are more interested to work in those areas in the hospital which will help them in their future venture. Often, they lack communication skill, and lack of communication, no communication, or the way they communicate with the patients and their attendants, particularly when the patient is sick, often becomes the reason of altercation with the attendants. There is nothing in the medical curriculum about the communication skill, which mostly comes with experience, and as that experience beingnaturally lacking, they become the most common target for argument with the patient’s relatives. I have no intention to question the competency of residents in care of patients, but in healthcare setup, one needs not only science of medicine but also art.
In view of long years of study before settling in life when compared to other streams, all India competition at every stage of career making it uncertain to get the next stage, reservation at every stage, and more-super specialization rather than family physician setup, it is not a surprise that many bright students are not opting medical profession in the country. With repeated violent behavior against doctor, it is not a surprise that younger generation is hesitant to take medical stream.
Despite so many hurdles, still the number of applicants for medical entrance examination in India has increased significantly in the past few years. Still it is considered a noble profession and expected to command a reasonable respect, which may get eroded if such frequent violent behavior continues against doctors by the public/relations of the patients. Furthermore, this respect has already been eroded due to the profession being taken under consumer protection act and demand and supply gap in infrastructure and human resource in healthcare sector.
Healthcare facility is a place where providing healthcare to patient is the combined effort of the teams involving doctors, nursing officer, hospital and sanitary attendants, laboratory persons under administrative supervision of policy makers like medical superintendent, head of the hospital, and administrator. However, whether it is emergency, regular inpatient ward, outpatient area, or procedure room, if there is any complication, fault, or mismanagement because of any team member, it is the doctor only who comes under attack by the patient’s attendant. Has any one of us seen the report that senior administrators or the owners are attacked by the relatives? The answer is big NO.
For India, one of the major drawbacks has been that health has never remained a priority for successive government since independence, without realizing that “healthy nation is a wealthy nation.” Public actors in the Indian healthcare system include the Ministry of Health and Family Welfare (MOHFW), state governments, and municipal and local bodies. Each state has its own Directorate of Health Services (DHS) and Department of Health and Family Welfare. District-level health services provide a link between each state and primary care services.
Other agencies involved in health system governance include the Insurance Regulatory and Development Authority, which regulates the health insurance industry, and the National eHealth Authority, which is to become the authority for development of an integrated health information system. There is lack of clarity in India with respect to which entities are responsible for regulating the private sector and for ensuring quality of care, as there are multiple agencies under different ministries.
For every lacuna in the system, a doctor is not to be blamed, and by no means any aggression against doctors is justified. It is the responsibility of lawmakers in the country that the rule of law should be upheld, and doctors can do their duties fearlessly.
Workplace violence in the ED is another pervasive issue in both the developed nations and India, with large numbers of physicians reporting having experienced various types of violence. Significant mental stress among ED practitioners is attributed to workplace violence, with potential financial impact to our institutions due to lost productivity of our ED workforce. While much work remains to decrease the incidence of workplace violence, it is critically important that institutional efforts are made to assist the ED workforce in coping with this common problem.
Violence in any form is not good for society. In backdrop of no established protocol for tackling such violence strict legislation, workplace management and reporting of violence should be in place. Further qualitative research studies on violence among other health-care providers and on patients and stakeholders’ perspectives on violence should also be considered.
If we want to end violence against doctors, we also need to change the attitudes of healthcare providers, avoid jousting in all forms, and engage with the patient community in every possible form relentlessly.
Patient partnership is changing medical practice across the world. A similar sea change is necessary in India. In a land where swamis and soothsayers make more television appearances than doctors, society needs a strong medical role model and a serious organization, may be somewhat like BMA in UK. We can take help of the media and other platforms to educate rather than sensationalize and give the medical profession an “image makeover.” Treatment can no longer be about “us and them.” No doctor enters a hospital with the intention of harming a patient, nothing can be learnt without making mistakes, and no outcome can be optimized in the face of limited facilities without co-operation and safety for themselves in mind. It is time that society understands this, and it is our job to explain it to them.
In conclusion it needs to be reiterated that attacks against healthcare providers deprive people of urgently needed care, endanger and demoralize health care providers, undermine health systems and long term public health goals, and contribute to the deterioration in the health and wellbeing of affected populations. For every health care professional who dies or flees, for every hospital that is destroyed, scores of people are denied health care. Each medical professional takes years of education and professional development— usually borne by the national budget— and supported by a family. Each hospital that is destroyed is a significant economic loss to the country. Let good sense and sanity prevail!
Disclaimer: The writer has taken help and excerpts of statements from WHO, few journals eg. BMJ as well as various publications on this subject sourced from the web.










Good writing but lengthy.
জনগণের জন্য এই লেখাটার বাংলা অনুবাদ চায়।